Introduction: The Hidden Core Revolution
For too long, women have suffered in silence with pelvic floor issues, believing symptoms like urinary leakage or pelvic pressure are simply “part of getting older.” This couldn’t be further from the truth.
According to the National Institutes of Health, pelvic floor disorders affect approximately one in four adult women in the United States. Yet despite this staggering prevalence, many women don’t know where to turn for help or even that effective treatments exist.
The American Urogynecologic Society (AUGS) emphasizes that pelvic floor disorders are highly treatable conditions, not inevitable consequences of aging. Understanding your body and accessing the right resources can transform your quality of life.
Breaking the Myth: It’s Not “Just Aging”
The belief that urinary leakage or prolapse is “just a normal part of aging” is a damaging misconception. While pelvic floor disorders (PFDs) are indeed highly prevalent—affecting roughly one in four adult women—they are not inevitable and are highly treatable. Research published in Scientific Reports confirms that while prevalence increases with age, proper intervention can significantly improve or resolve symptoms at any stage of life.
What Exactly Is the Pelvic Floor?
The pelvic floor is more than just a set of muscles—it’s a complex system that acts as a supportive foundation for your body. Imagine a hammock stretched across the bottom of your pelvis, holding up your bladder, uterus, and bowel. This “hammock” also plays crucial roles in:
- Bladder and bowel control through sphincter function
- Sexual function and sensation
- Core stability during movement
- Postural support in coordination with your deep abdominal muscles
Why the Pelvic Floor Changes After 40
The years leading into and following menopause mark a critical turning point. Declining estrogen levels affect the strength and elasticity of all tissues in the pelvis, making women more susceptible to pelvic floor disorders. This hormonal vulnerability, combined with decades of cumulative strain from childbirth, chronic cough, or heavy lifting, necessitates a focused approach to care.
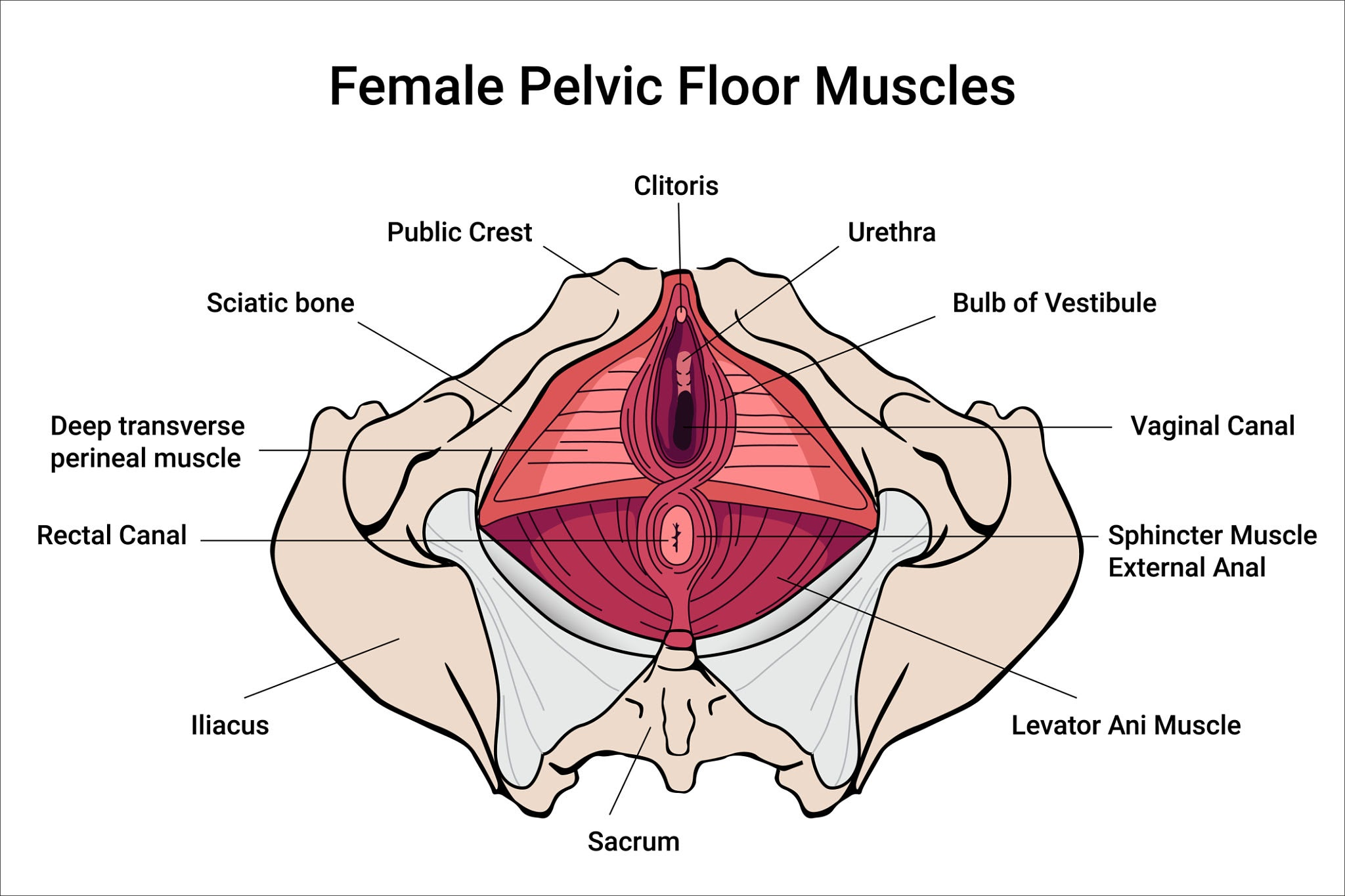
Understanding Your Pelvic Floor: Anatomy 101
Before diving into solutions, it’s essential to understand what’s happening beneath the surface. The International Continence Society provides extensive educational resources on pelvic anatomy, helping women visualize this often-misunderstood area of the body.
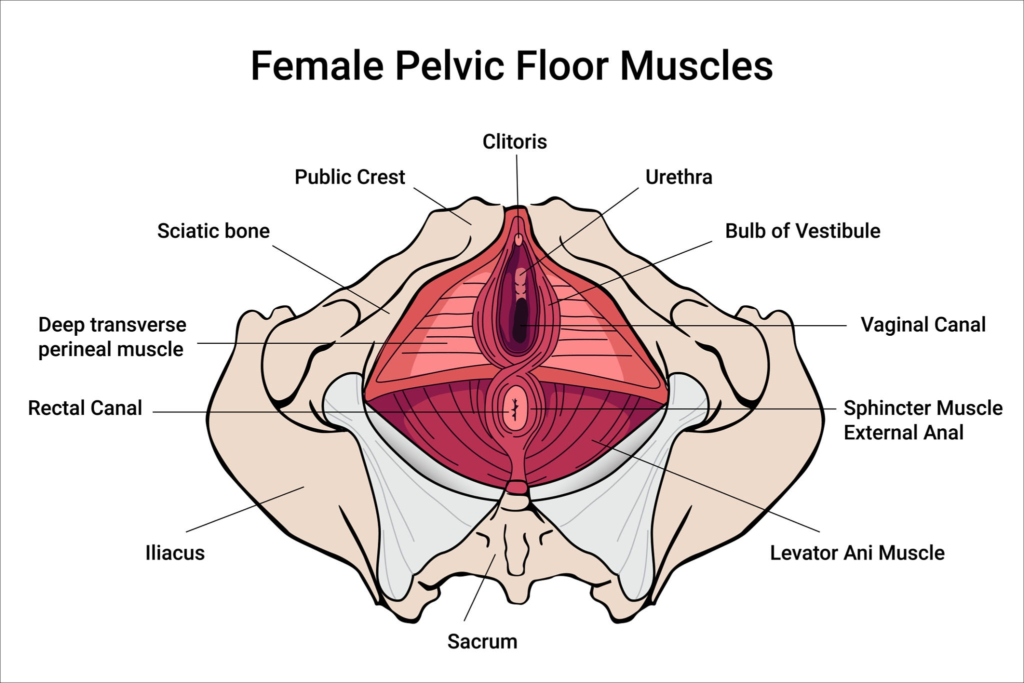
The Deep Support System
The pelvic floor consists of several layers of muscles working in concert:
The Levator Ani forms the deeper layer, providing structural support and stability for your pelvic organs. Think of this as the primary “floor” holding everything in place.
The Superficial Layer includes muscles that control the urethral and anal sphincters, helping with bladder and bowel function. These are your body’s natural “gatekeepers.”
The Inner Core Connection
Your pelvic floor doesn’t work alone—it’s part of a larger team that forms the “Inner Core.” According to research featured by the Continence Foundation of Australia, this system includes:
- The diaphragm (your breathing muscle)
- The transverse abdominis (deep abdominal muscles)
- The multifidus (small stabilizing muscles in your back)
- The pelvic floor muscles
When healthy, the pelvic floor coordinates with the diaphragm like a piston—moving gently down on inhale and up on exhale to maintain balance, pressure management, and posture.
Understanding Intra-Abdominal Pressure (IAP)
Every time you cough, sneeze, lift a heavy object, or laugh, your body creates Intra-Abdominal Pressure (IAP). When the pelvic floor is functioning optimally, it automatically contracts to counteract this pressure. When compromised, IAP pushes downward, contributing directly to symptoms like urinary leakage or pelvic organ prolapse.
Common Pelvic Floor Disorders After 40
The Mayo Clinic and Cleveland Clinic both maintain comprehensive databases on pelvic floor disorders. Here are the most common conditions affecting women over 40:
Urinary Incontinence (UI)
The involuntary loss of urine is the most frequently reported pelvic floor disorder, affecting millions of women worldwide. Click here for detailed information on urinary incontinence
Stress Incontinence (SUI) occurs when physical activities that increase abdominal pressure—coughing, sneezing, jumping, or even laughing—cause urine leakage. This happens when the pelvic floor muscles can’t adequately support the bladder neck during these pressure spikes.
Urge Incontinence (Overactive Bladder) is characterized by a sudden, intense urge to urinate that’s difficult to postpone, sometimes leading to accidental leakage before reaching the bathroom.
Many women experience mixed incontinence, a combination of both stress and urge symptoms.
Pelvic Organ Prolapse (POP): The Feeling of Heaviness
Pelvic organ prolapse occurs when the connective tissues and muscles become too weak to fully support the organs, causing them to descend into the vaginal canal. According to the American College of Obstetricians and Gynecologists (ACOG), symptoms often include:
- A feeling of heaviness or pressure in the pelvis
- A bulge or protrusion in the vaginal area
- Lower back discomfort
- Difficulty with bowel movements or urination
Common types include:
- Cystocele (bladder prolapse)
- Uterine prolapse (uterus descending)
- Rectocele (rectum bulging forward)
While prolapse can feel intimidating, it’s a manageable condition that often improves significantly with conservative care.
The Pain and Tightness Paradox: Hypertonicity
Not all pelvic floor disorders stem from weakness. High-tone pelvic floor dysfunction (HTPFD) or hypertonicity is characterized by muscles that are constantly in a state of tension or tightness.
Symptoms include:
- Chronic pelvic pain
- Pain during intercourse (dyspareunia)
- Difficulty emptying the bladder or bowels
- Painful urination
- Lower back pain
For women with hypertonicity, traditional strengthening exercises like Kegels can actually worsen symptoms. This is why proper assessment is crucial before beginning any exercise program.
The Menopause Effect: When Hormones Meet Structure
The North American Menopause Society (NAMS) provides extensive research on how hormonal changes impact pelvic health.
Estrogen’s Critical Role
Estrogen is essential for maintaining the health of tissues throughout the pelvis. It supports:
- Collagen production in ligaments and fascia
- Tissue thickness and elasticity
- Moisture in vaginal tissues
- Blood flow to the pelvic region
As estrogen declines during perimenopause and menopause, these tissues undergo significant changes. The supporting fascia and ligaments lose elasticity and become thinner, compromising the structural “anchors” that hold pelvic organs in place. This leaves the muscles bearing an even heavier load.
Genitourinary Syndrome of Menopause (GSM)
GSM is the clinical term for the constellation of symptoms caused by estrogen deficiency, as defined by the International Society for the Study of Women’s Sexual Health (ISSWSH):
- Vaginal dryness and thinning
- Discomfort or pain during intercourse
- Urinary urgency and frequency
- Recurrent urinary tract infections
- Decreased lubrication
These tissue changes directly impact sexual function and increase the likelihood of urinary issues, creating a cascade effect that diminishes quality of life.
Lifestyle Accelerants
Decades of repeated pressure create cumulative wear-and-tear:
Chronic straining from long-term constipation forces IAP downward, greatly increasing the risk of prolapse over time.
High-impact activities like running or jumping without proper muscular bracing place continuous strain on supporting tissues, particularly if begun without adequate preparation.
Chronic coughing from smoking, asthma, or allergies creates repeated IAP spikes that stress the pelvic floor thousands of times over the years.
Evidence-Based Solutions: What Actually Works
Myth-Busting: Why “Just Do Kegels” Isn’t Enough
The advice to “just do Kegels” is oversimplified and potentially harmful. Generic Kegels are ineffective if:
- You’re performing them incorrectly (studies show up to 30% of women cannot correctly contract their pelvic floor without guidance)
- Your muscles are already hypertonic (tight)
- You have coordination issues rather than weakness
- You’re bearing down instead of lifting up
For high-tone pelvic floor dysfunction, relaxation and manual release are the necessary first steps, not strengthening.
The Gold Standard: Pelvic Floor Physical Therapy (PFPT)
PFPT is recognized by the American Physical Therapy Association (APTA) as a conservative, first-line treatment for most pelvic floor disorders. A trained pelvic floor physical therapist performs an individualized internal and external assessment to determine the root cause—whether weakness, tightness, coordination issues, or a combination.
Treatment includes:
- Biofeedback technology to visualize muscle function
- Manual techniques to release tension and trigger points
- Personalized exercise programs
- Education on pressure management and body mechanics
- Breathing coordination training
To find a qualified therapist, visit the American Physical Therapy Association’s directory or search through Herman & Wallace Pelvic Rehabilitation Institute.
Correct Pelvic Floor Muscle Training (PFMT)
When strengthening IS indicated after proper assessment, training must target both fiber types:
Slow-Twitch Endurance Holds: Contracting for sustained periods (5-10 seconds) builds postural support. These muscles need stamina to support your organs throughout the day.
Fast-Twitch Quick Contractions: Short, sharp contractions (1-2 seconds) quickly close the sphincters to “catch” a sudden leak during a cough or sneeze.
Critical Component—Full Relaxation: The muscle must be allowed to fully lengthen and relax between contractions. This is just as important as the contraction itself and prevents the development of hypertonicity.
Mastering “The Knack”: Your Safety Net
“The Knack” is an anticipatory reflex technique that involves contracting and lifting the pelvic floor just before and during a sudden increase in IAP—before you cough, sneeze, or laugh. This evidence-backed strategy, documented in research from the Journal of Urology, can significantly prevent leakage in high-pressure moments.
How to practice:
- Feel a cough or sneeze coming
- Quickly contract your pelvic floor (imagine stopping the flow of urine)
- Hold through the cough/sneeze
- Release and relax afterward
Essential Products and Tools for Pelvic Floor Health
The right tools can significantly enhance your pelvic floor health journey. Here are evidence-based products recommended by pelvic health specialists:
For Bowel Health and Proper Positioning
Squatty Potty Toilet Stool — This medical-grade toilet stool achieves the optimal 35-degree squatting angle that naturally relaxes the puborectalis muscle sling, eliminating straining during bowel movements. Chronic straining is one of the primary contributors to prolapse, making this simple tool remarkably effective for prevention.
For Pelvic Floor Relaxation and Release
Intimate Rose Pelvic Wand — For women diagnosed with hypertonicity by their pelvic floor physical therapist, a therapeutic pelvic wand can aid in releasing painful trigger points under professional guidance. This tool should only be used after assessment and instruction from a qualified PFPT.
For Biofeedback and Training
Elvie Trainer or Pericoach — These FDA-approved biofeedback devices connect to smartphone apps, providing real-time feedback on pelvic floor contractions. They help ensure you’re performing exercises correctly and can track progress over time. Particularly useful for women who struggle with proper muscle engagement.
For Tissue Health
Vitamin E Suppositories and Hyaluronic Acid Moisturizers — For vaginal dryness and tissue thinning, products like Replens or hyaluronic acid-based vaginal moisturizers can provide relief between doctor visits. However, these should complement, not replace, conversations with your physician about prescription vaginal estrogen therapy.
Holistic Lifestyle Modifications
Optimizing Bowel and Bladder Habits
Eliminate straining by maintaining a high-fiber diet (25-35 grams daily) and adequate hydration (aim for pale yellow urine). The Academy of Nutrition and Dietetics recommends gradually increasing fiber intake while drinking plenty of water.
Establish a bathroom routine without forcing. Never “just in case” urinate frequently, as this can train your bladder to hold less volume over time.
Use proper positioning with a toilet stool to achieve the optimal squatting angle that relaxes the pelvic floor during bowel movements.
Smart Exercise Choices
The International Urogynecological Association emphasizes the importance of exercise modification during pelvic floor recovery:
Avoid temporarily:
- High-impact activities (running, jumping)
- Heavy lifting without proper bracing
- Traditional crunches or sit-ups that increase IAP
- Exercises that create a “doming” or bulging in the abdominal wall
Embrace instead:
- Swimming and water aerobics
- Cycling with proper posture
- Walking with attention to core engagement
- Pilates or yoga with pelvic floor modifications
- Strength training with proper breathing and bracing
Supportive Medical Therapies
Topical Vaginal Estrogen: Local estrogen therapy is highly effective for restoring thickness and elasticity to vaginal and urinary tissues affected by GSM. According to the Mayo Clinic, vaginal estrogen has minimal systemic absorption and excellent safety profiles. Products include creams (Estrace, Premarin), tablets (Vagifem), or rings (Estring). Discuss options with your physician or gynecologist.
Hormone Replacement Therapy (HRT): For some women, systemic hormone therapy may be appropriate. The North American Menopause Society provides evidence-based guidance on HRT benefits and risks.
When to Seek Professional Help
Don’t wait until symptoms become severe. Consider consulting a specialist if you experience:
- Any urinary leakage during daily activities
- A feeling of heaviness or bulge in the pelvic area
- Painful intercourse or pelvic pain
- Difficulty emptying your bladder or bowels
- Recurrent urinary tract infections
Finding the Right Providers
Pelvic Floor Physical Therapist (PFPT): Search the APTA directory or Herman & Wallace Pelvic Rehabilitation Institute
Urogynecologist: Board-certified specialists in female pelvic medicine and reconstructive surgery. Find one through AUGS
Urologist specializing in female urology: Search through the American Urological Association
Your Action Plan: Take Control of Your Core
Pelvic floor disorders are common, but they are absolutely not an inevitable part of aging. With knowledge, proper care, and the right resources, you can take proactive steps to protect and improve your core foundation.
Start Today:
- Schedule an assessment with a pelvic floor physical therapist, even if you’re not currently experiencing symptoms
- Invest in a toilet stool to eliminate straining during bowel movements
- Talk to your doctor about vaginal estrogen therapy if you’re experiencing menopausal symptoms
- Modify your exercise routine to protect your pelvic floor during recovery
- Practice “The Knack” during daily activities that increase pressure
Remember: seeking help is a sign of strength, not weakness. Your pelvic floor has supported you through decades of life—now it’s time to support it back.
Evidence-Based Resources and Citations
Research Sources:
- Kenne, K. A. et al. Prevalence of pelvic floor disorders in adult women being seen in a primary care setting and associated risk factors. Scientific Reports. 2022; 12(1): 1-10. PubMed
- Al-Ghorani, H. et al. Pelvic floor dysfunction: prevalence and associated factors. BMC Women’s Health. 2023; 23(1): 1-12. Full Text
- De Oliveira, C. E. et al. Pelvic floor physical therapy in the treatment of pelvic floor dysfunction in women. Current Opinion in Urology. 2019; 29(5): 421–425. Stanford Medicine
- Mayo Clinic Staff. Vaginal atrophy (Genitourinary Syndrome of Menopause). Mayo Clinic
- Pinpoint Physiotherapy. Pelvic Floor Dysfunction, Assessment, & Treatment. Resource
- Torosis, M. et al. A Treatment Algorithm for High-Tone Pelvic Floor Dysfunction. AUGS Fact Sheet. PubMed
- Varghese, T. M. Pelvic floor physical therapy in the treatment of pelvic floor dysfunction in women. Indian Journal of Urology. 2019; 35(3): 161–162. PubMed
Authoritative Organizations:
- American Urogynecologic Society (AUGS): www.augs.org
- American Physical Therapy Association: www.apta.org
- North American Menopause Society: www.menopause.org
- International Continence Society: www.ics.org
- Mayo Clinic Pelvic Health: www.mayoclinic.org
This guide is regularly updated with the latest research and clinical findings. Bookmark this page as your comprehensive resource for pelvic floor health throughout midlife and beyond.