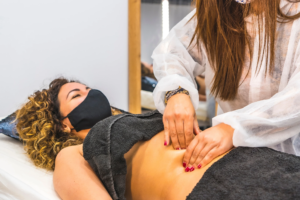
If you’ve noticed unexpected leaks when you laugh, sneeze, or rush to the bathroom, you’re far from alone.”Nearly 50% of adult women experience urinary incontinence, with prevalence increasing to up to 75% of women over 65.”
Despite how common it is, many women suffer in silence, believing it’s just an inevitable part of aging. The truth? Incontinence (bladder leakage) is treatable, and healthcare providers can help figure out the cause of bladder control issues.
For the broad context on pelvic changes in menopause, we recommend this article: Your Complete Guide to Menopause, Bladder Health, and Pelvic Floor Wellness.
What Is Incontinence?
Urinary incontinence is when you lose control of your bladder and leak pee. It can range from occasional small leaks to more significant loss of bladder control. While it becomes more common as we age, it’s not a normal part of aging that you simply have to accept.
Types of Incontinence You Should Know About

Understanding what type of incontinence you’re experiencing is the first step toward finding the right solution.
Quick Reference: Which Type Do I Have?
| Type | Trigger | What It Feels Like |
|---|---|---|
| Stress | Coughing, sneezing, exercise | Small leaks with physical pressure |
| Urge | Sudden need to go | Can’t make it to bathroom in time |
| Mixed | Both triggers | Combination of above |
| Overflow | Constant | Frequent dribbling, never feel empty |
Stress Incontinence
This is the most common type among women, especially after childbirth or during menopause. Stress incontinence is defined as the complaint of involuntary loss of urine on effort or physical exertion, such as sporting activities, or on sneezing or coughing.
You might leak a few drops when you lift something heavy, exercise, or even just walk or stand up quickly in more advanced cases. The term “stress” refers to physical pressure on your bladder, not emotional stress.
Urge Incontinence (Overactive Bladder)
This type involves a sudden, intense urge to urinate that’s difficult to control. Urge incontinence is the sudden urge to go to the bathroom that’s so severe that people may leak on the way to the bathroom. You might find yourself rushing to the bathroom frequently throughout the day and night, and sometimes you don’t make it in time.
Mixed Incontinence
Many women experience a combination of both stress and urge incontinence. This is called mixed incontinence and requires addressing both components for effective treatment.
Overflow Incontinence
This occurs when your bladder doesn’t empty completely, resulting in frequent dribbling or a continuous small leak. You might feel like you can never fully empty your bladder.
Why Does This Happen to Women Over 40?
Several factors contribute to incontinence in women, and many become more prominent as we age.
Hormonal Changes and Menopause
The connection between menopause and bladder control is significant and often overlooked. According to Cleveland Clinic, your hormones, especially estrogen, change during menopause, which can affect how you can control your bladder.”
The lower genital and lower urinary tract share similar embryologic origin and contain abundant estrogen receptors.
As estrogen levels decline during perimenopause and menopause, these tissues can become weaker and less elastic.
Estrogen helps maintain the strength and flexibility of the muscles surrounding the bladder and pelvic organs, but as levels drop significantly during menopause, the urethral and vaginal tissues may become thinner.
This is why the loss of estrogen affects so many aspects of your urinary and pelvic health.
Childbirth
Physical changes from pregnancy, childbirth, or menopause can result in stress incontinence. Pregnancy and vaginal delivery can weaken or damage the pelvic floor muscles and nerves that support bladder control.
Even women who had cesarean sections may experience some weakening due to the weight and pressure of pregnancy itself.
Weight and Lifestyle Factors
Carrying extra weight puts additional pressure on your bladder and pelvic floor muscles, which can worsen incontinence or increase your risk of developing it.
Caffeine prompts your body to get rid of fluids, which causes you to need to urinate, and the acids in carbonated drinks and some foods can irritate your bladder.
Other Contributing Factors
Chronic coughing, constipation, certain medications, urinary tract infections, and nerve damage from conditions like diabetes can all contribute to bladder control issues.
What Can You Do About It?
The good news is that incontinence is highly treatable. Most women see significant improvement with conservative treatments, and you have many options to explore.
Pelvic Floor Exercises (Kegels)

These exercises are often the first line of defense and can be remarkably effective. According to Johns Hopkins Medicine, exercise can help strengthen or relax pelvic floor muscles through pelvic floor therapy.”. Kegel exercises work by strengthening the muscles that support your bladder and urethra.
How to Do Kegel Exercises Correctly:
Find the right muscles: The easiest way is to imagine you’re trying to stop urinating midstream or prevent passing gas. Those are your pelvic floor muscles. Don’t actually stop your urine flow regularly, as this can lead to incomplete bladder emptying.
Perfect your technique: Make sure your bladder is empty, then sit or lie down. Tighten your pelvic floor muscles. Hold tight and count 3 to 5 seconds. Relax the muscles and count 3 to 5 seconds. Make sure you’re not tightening your stomach, thighs, or buttocks.
Build up gradually: Start with 10 repetitions, three times a day. As you get stronger, work up to holding for 10 seconds with 10-second rest periods between contractions.
Be patient and consistent: After 4 to 6 weeks, you should have fewer symptoms. The key is making these exercises a lifelong habit.
Important note: If you’re unsure whether you’re doing Kegels correctly, consider consulting a pelvic floor physical therapist. Johns Hopkins Physical Medicine and Rehabilitation offers personalized, one-on-one physical therapy sessions in a private setting tailored to your symptoms and health goals.
Many women find biofeedback devices helpful for learning correct technique at home. These devices provide real-time confirmation that you’re contracting the right muscles—studies show that up to 60% of women perform Kegels incorrectly without feedback. See our complete guide to choosing the best Kegel trainer for your needs, including 6 devices tested specifically for women over 40.
Lifestyle Modifications
Simple changes can make a significant difference:
Manage your weight: Even a modest weight loss of 5-10% can improve symptoms.
Watch your fluid intake: Stay hydrated but avoid excessive fluids before bed. Contrary to what you might think, restricting fluids too much can actually irritate your bladder by making urine more concentrated.
Limit bladder irritants: Reduce caffeine, alcohol, carbonated beverages, artificial sweeteners, and acidic foods like citrus and tomatoes.
Address constipation: Straining puts pressure on your pelvic floor. Increase fiber and stay hydrated.
Quit smoking: Chronic coughing from smoking can worsen stress incontinence.
Bladder Training
This technique involves gradually increasing the time between bathroom visits to help your bladder hold more urine. You start by urinating on a schedule rather than whenever you feel the urge, then slowly extend the intervals between visits.
Hormone Therapy
Research from Cleveland Clinic and other leading institutions shows that local hormone treatment can restore bladder function. Vaginal estrogen therapy, administered via creams or rings, delivers estrogen directly to the vaginal area, effectively alleviating symptoms of urgency, frequency, and stress incontinence.
This is different from systemic hormone replacement therapy. Estrogen improves the elasticity and the strength of the muscles in the pelvic floor thereby expanding bladder control and raises the bladder’s sensory threshold thereby reducing urinary incontinence.
Local estrogen specifically helps restore tissue health, thickness, and elasticity in the vaginal and urethral areas, which can significantly improve bladder control symptoms.
For optimal results, many healthcare providers recommend pairing vaginal estrogen with regular vaginal moisturizers to maintain tissue health between applications. Understanding the difference between moisturizers (which restore tissue moisture long-term) and lubricants (which provide temporary comfort) can help you choose the right products. Learn the difference between vaginal moisturizers and lubricants and which you need for menopausal symptoms.
Medications
Depending on your type of incontinence, several medications can help:
For urge incontinence: Anticholinergics help relax your bladder, and Beta 3 agonist medications relax the bladder muscle and can increase the amount of urine your bladder can hold.
For stress incontinence: Some medications can help strengthen the urethral sphincter.
Your healthcare provider will discuss potential benefits and side effects with you.
Physical Devices
Several devices can provide support:
Pessaries: Pessary is a silicone-based device that is fitted to the vagina and inserted by a healthcare professional, with knob present in incontinence ring pessaries pushing on the urethra to overcome stress pressure. Pessaries come in different sizes and styles, and proper fitting by a healthcare professional is essential.
Urethral inserts: Small disposable devices that temporarily plug the urethra to prevent leakage during specific activities.
Medical Procedures
When conservative treatments aren’t sufficient, various procedures can help:
Botox injections: For severe symptoms, bladder muscle Botox injections offer reasonable improvements in symptoms for six months or longer.
Nerve stimulation: Peripheral tibial nerve stimulation uses an acupuncture-like needle and mild electric simulation, while sacral nerve modulation is a surgical implantation of a device that helps modulate neuronal circuitry.
Surgery: According to Mayo Clinic, studies show that over 77% of women with stress urinary incontinence are cured or have significant improvements lasting up to 11 years after midurethral sling surgery.
When Should You See a Doctor?
You should consult with a healthcare provider if:
- Incontinence is affecting your daily activities, exercise, or social life
- You’re avoiding activities you enjoy because of leakage concerns
- You’re experiencing pain during urination
- You notice blood in your urine
- Conservative measures haven’t helped after several weeks
- Your symptoms suddenly worsen
Don’t feel embarrassed about discussing this with your doctor. According to Mayo Clinic specialists, urine incontinence is common and effective treatments are available. Your healthcare provider has likely helped hundreds of women with similar concerns.
Living Well with Incontinence
While you work on improving your symptoms, several strategies can help you maintain your quality of life:
Practical Tips
Wear absorbent pads or protective underwear when needed. Today’s products are discreet, comfortable, and highly effective.
Map out bathrooms when you’re going somewhere new.
Do a Kegel before you sneeze, cough, or lift something heavy to help prevent leaks.
Wear dark-colored or patterned clothing if you’re concerned about visible leaks.
Keep a spare change of clothes in your car or bag for peace of mind.
Stay Active

Don’t let incontinence stop you from exercising. Physical activity is crucial for overall health and can actually help improve incontinence by helping with weight management and strengthening core muscles. Consider:
- Wearing a pad or liner during exercise
- Emptying your bladder before working out
- Doing a few Kegels before and during exercise
- Choosing low-impact activities if high-impact exercise causes significant leakage
Maintain Social Connections
Isolation can lead to depression and decreased quality of life. Stay connected with friends and family. Remember, millions of women are dealing with the same issue, and chances are some of your friends are too.
Your Next Steps: Taking Action
Now that you understand what’s causing your symptoms, here are concrete next steps:
If you’re ready to start Kegel exercises: Not sure if you’re doing them correctly? This comprehensive guide to Kegel trainers reviews 6 biofeedback devices that provide real-time feedback, from budget-friendly options starting at $49 to clinical-grade devices. Each device is evaluated for women over 40 dealing with menopausal symptoms.
If vaginal dryness is part of your symptoms: Declining estrogen affects both bladder control and vaginal tissue health. Learn which moisturizers and lubricants work best for menopausal symptoms and how to combine them with hormone therapy for optimal results.
If you’re preparing for a doctor visit: Keep a bladder diary for 3-7 days before your appointment, tracking when leaks occur, what you were doing, and how much fluid you’re drinking. This gives your provider valuable information for diagnosis.
If you want comprehensive pelvic floor information: Read our complete guide to menopause, bladder health, and pelvic floor wellness for the full picture of how these systems work together and affect your quality of life during perimenopause and beyond.
Common Questions and Concerns
Will it get worse with age?
Not necessarily. While the risk increases with age, taking proactive steps now, particularly with pelvic floor exercises and maintaining a healthy lifestyle, can prevent worsening and may even reverse symptoms.
Is surgery my only option?
Absolutely not. Surgery is typically reserved for cases that don’t respond to conservative treatments. Most women see significant improvement with lifestyle changes, pelvic floor exercises, and other non-surgical approaches.
Can men have this problem too?
Yes, though it’s less common in men. When it does occur, it’s often related to prostate issues or surgery.
How long does treatment take?
For pelvic floor exercises, you may start noticing improvement within 4-6 weeks of consistent practice. Other treatments work at different speeds, so patience and persistence are important.
Will my sex life be affected?
Incontinence can impact intimacy, but many treatments actually improve sexual function. Strong pelvic floor muscles can enhance sensation and make orgasm easier to achieve. Additionally, treating incontinence can boost confidence and reduce anxiety about intimacy.
Frequently Asked Questions
What is the main cause of urinary incontinence in women over 40?
The primary cause is declining estrogen during menopause, which weakens pelvic floor muscles and urethral tissues. Childbirth, weight gain, and chronic conditions also contribute. Most cases respond well to pelvic floor exercises and lifestyle modifications.
How long does it take for Kegel exercises to work?
Most women notice improvement within 4-6 weeks of consistent daily practice. The key is performing them correctly—many women unknowingly use the wrong muscles. Biofeedback devices can help ensure proper technique.
Is bladder leakage a normal part of aging?
No. While incontinence becomes more common with age, it’s a treatable medical condition, not an inevitable part of getting older. Up to 80% of women see significant improvement with appropriate treatment.
Should I see a doctor for minor leakage?
Yes, especially if it’s affecting your quality of life or preventing you from activities you enjoy. Early intervention often leads to better outcomes, and your doctor can rule out underlying conditions.
Can menopause cause sudden urge to urinate?
Yes. Declining estrogen affects bladder sensitivity and can trigger overactive bladder symptoms, including sudden urgent needs to urinate. This is called urge incontinence and is very common during perimenopause and menopause.
Will losing weight help with incontinence?
Yes. Studies show that losing just 5-10% of body weight can reduce incontinence episodes by up to 50%. Extra weight puts additional pressure on the bladder and pelvic floor muscles.
The Bottom Line
Female stress urinary incontinence is a common diagnosis, occurring in 26% to 49% of women, and can significantly impact a patient’s quality of life. But it doesn’t have to control your life.
From simple pelvic floor exercises to hormone therapy and medical procedures, numerous effective treatments exist. The most important step is talking to your healthcare provider and starting treatment early, before symptoms worsen.
Remember, incontinence isn’t a character flaw or something to be ashamed of. It’s a medical condition with medical solutions. With the right approach, most women can significantly improve or even eliminate their symptoms.
You deserve to laugh without worry, exercise without fear, and live your life fully. Take that first step and talk to your doctor. Better days are ahead.
References
Mayo Clinic. (2023). Urinary incontinence – Symptoms and causes
Mayo Clinic. (2023). Urinary incontinence – Diagnosis and treatment
Mayo Clinic Health System. (2023). Is urine incontinence normal for women?
Mayo Clinic Health System. (2025). Is incontinence in women treatable?
Cleveland Clinic. (2025). Urinary Incontinence: Causes, Leakage, Types & Treatment
Johns Hopkins Medicine. (2025). Pelvic Floor Therapy
Johns Hopkins Physical Medicine and Rehabilitation. Pelvic Floor Therapy
National Institutes of Health. Pre- versus Post-Menopausal Onset of Overactive Bladder and the Response to Vaginal Estrogen Therapy
This article provides general health information and should not replace professional medical advice. Always consult with your healthcare provider about your specific situation and treatment options.